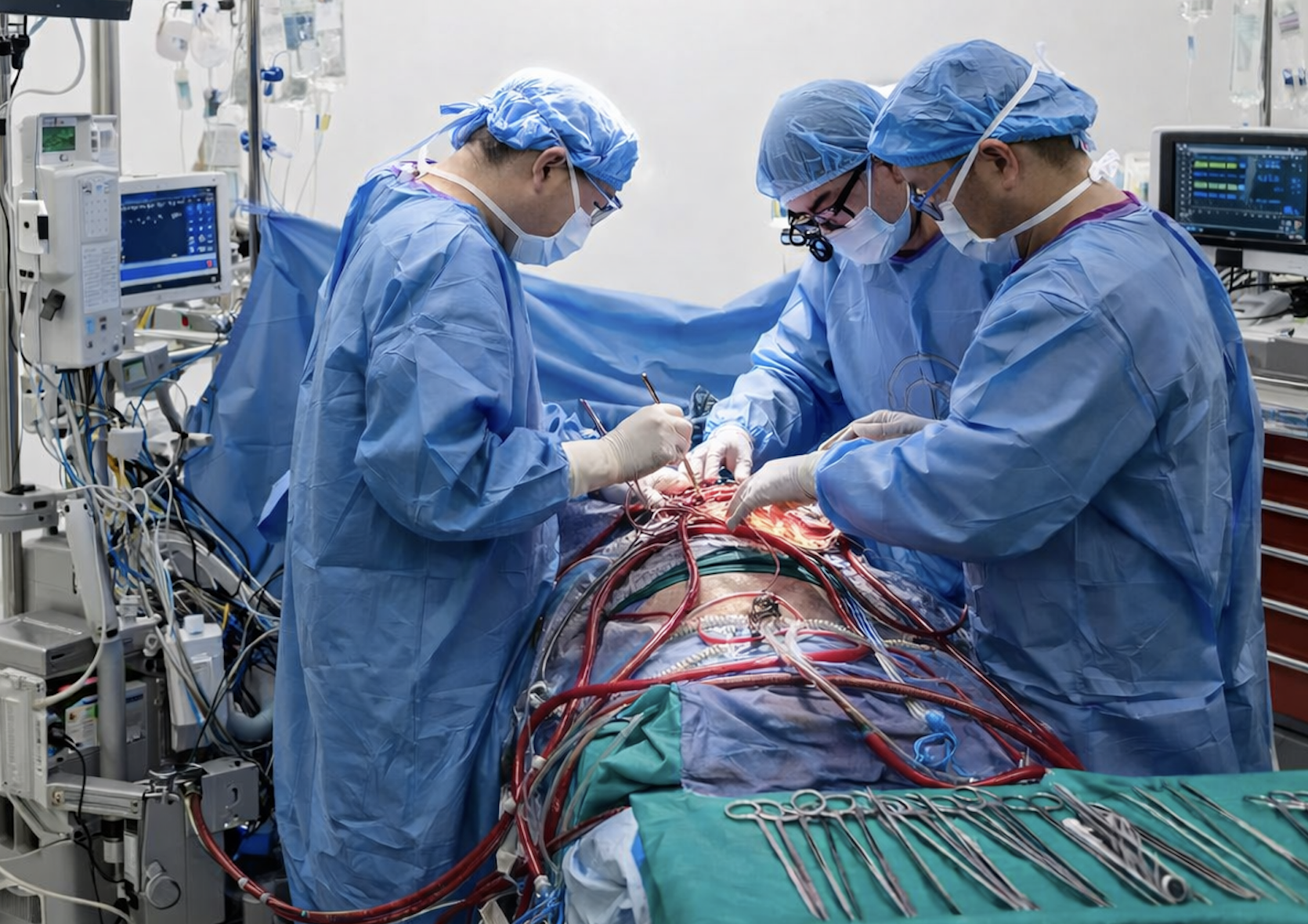
Extracorporeal Membrane Oxygenation (ECMO) is continually emerging as an increasingly vital therapy for critically ill patients. As more healthcare institutions recognize the life-saving potential of ECMO and establish programs to meet growing demand, a critical question emerges: How can ICU teams maintain the specialized expertise required to deliver exceptional ECMO care consistently?
The answer lies in comprehensive, ongoing ECMO education that extends far beyond initial program training. For ICUs committed to delivering the highest standard of critical care, investing in continuous ECMO education is more than beneficial—it’s essential.
The Reality of ECMO Skill Maintenance
ECMO represents one of the most complex therapies in modern medicine, requiring practitioners to master intricate technical skills, sophisticated clinical decision-making, and rapid response capabilities. Unlike many ICU procedures that staff encounter daily, ECMO cases may be infrequent at many facilities, creating a unique challenge: how to maintain proficiency when regular practice opportunities are limited.
Research consistently demonstrates that technical skills decline without regular use—a phenomenon known as skill decay. In the high-stakes world of ECMO care, where split-second decisions can determine patient outcomes, this reality poses significant risks to both patient safety and program effectiveness.
Consider the typical scenario: an ICU team receives excellent initial ECMO training, successfully launches their program, and begins caring for patients. However, if ECMO cases remain sporadic—perhaps only a handful per year—team members may find their confidence and competency gradually diminishing between cases. When the next ECMO patient arrives, that hesitation or uncertainty could prove costly.
Beyond Initial Training: The Continuing Education Imperative
While comprehensive initial training provides the foundation for ECMO competency, the dynamic nature of this field demands ongoing education that keeps pace with evolving best practices, emerging technologies, and refined protocols. ECMO guidelines and techniques continue to advance, with new evidence shaping everything from cannulation strategies to weaning protocols.
Successful ECMO programs recognize that education must be viewed as a continuous process rather than a one-time event. This ongoing commitment to learning serves multiple critical functions:
- Combating Skill Decay: Regular refresher training and competency assessments help maintain the sharp technical skills essential for ECMO success, even during periods of low case volume.
- Staying Current: The ECMO field evolves rapidly, with new research influencing best practices and protocols. Ongoing education ensures teams remain at the forefront of evidence-based care.
- Building Confidence: Regular practice and education build the confidence necessary for teams to respond decisively in critical moments, reducing hesitation that could impact patient outcomes.
- Ensuring Consistency: Continuous education helps maintain standardized approaches across all team members, reducing variability in care delivery.
The Business Case for ECMO Education Investment
Beyond the obvious clinical benefits, ongoing ECMO education delivers measurable value to healthcare institutions as well:
- Improved Patient Outcomes: Well-trained teams demonstrate better patient survival rates, shorter ECMO runs, and fewer complications—outcomes that directly translate to improved quality metrics and patient satisfaction scores.
- Enhanced Revenue Optimization: ECMO represents one of the highest DRG reimbursement in healthcare today, offering significant revenue potential. However, complications, extended runs, or suboptimal coding can impact these financial benefits. Continuous education helps ensure teams deliver efficient, effective care while maximizing appropriate reimbursement.
- Risk Mitigation: Comprehensive, ongoing training reduces the likelihood of adverse events, helping protect both patients and institutions from potential liability issues.
- Staff Retention and Satisfaction: Healthcare professionals value opportunities for continued learning and skill development. Investing in ongoing ECMO education demonstrates institutional commitment to staff growth, potentially contributing to improved retention rates.
- Program Reputation: Institutions known for excellence in ECMO care attract referrals, enhance their reputation as regional centers of excellence, and may be better positioned for quality recognition programs.
A Multifaceted Approach to Ongoing ECMO Education
Effective ongoing ECMO education requires a comprehensive approach that accommodates diverse learning styles, busy schedules, and varying levels of experience. The most successful programs combine multiple educational modalities:
Structured Online Learning
Online platforms provide convenient access to updated protocols, case studies, and theoretical foundations. This format allows team members to learn at their own pace while ensuring consistent, standardized content delivery across the entire team.
High-Fidelity Simulation
Regular simulation sessions using actual ECMO equipment provide hands-on practice opportunities that mirror real-world scenarios. These sessions help teams practice both routine procedures and emergency situations in a safe, controlled environment.
Competency Assessments
Regular evaluations help identify knowledge gaps and ensure all team members maintain required proficiency levels. These assessments also provide documentation for credentialing and quality assurance purposes.
Bedside Precepting
Working alongside experienced ECMO specialists during actual patient care provides the most authentic learning experience possible. This real-world mentorship allows teams to apply their knowledge in live clinical situations while receiving immediate guidance, feedback, and expert insight. The transition from simulation to actual bedside care with expert support builds confidence and competence that cannot be replicated in any other educational format.
The Path Forward: Making ECMO Education a Strategic Priority
The most successful ECMO programs treat education as a strategic investment, knowing that exceptional education benefits the clinicians, patients, and institution as a whole. They recognize that in the complex world of ECMO care, knowledge and skills represent their most valuable assets—assets that require ongoing maintenance and enhancement to deliver optimal value.
As the demand for ECMO therapy continues to grow and patient acuity increases, the institutions that thrive will be those that commit to continuous learning and improvement. By investing in comprehensive, ongoing ECMO education, ICUs can ensure they’re prepared to meet whatever challenges the future may bring.
Your patients’ lives depend on it. Your team’s success depends on it. Your program’s future depends on it.
Isn’t it time to make ongoing ECMO education the strategic priority it deserves to be?