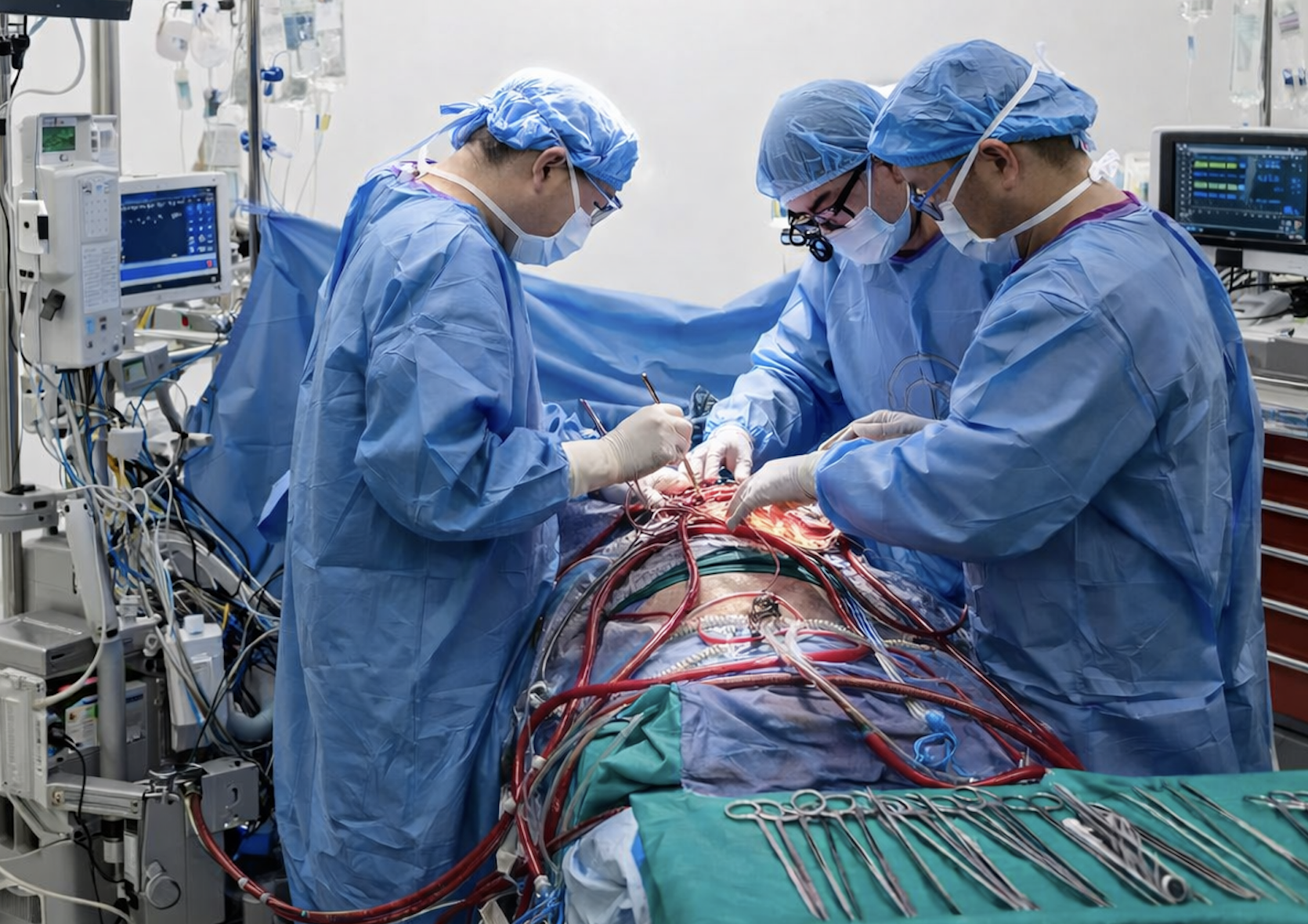
Building an ECMO program looks different on paper than it does in practice. After years of supporting program launches across the country, we’ve learned that success often hinges on factors that aren’t always obvious at the outset.
With the Bridging Life Critical Care Symposium coming up next week in Houston, we’ve been connecting with hospital partners about lessons learned and the things they wish someone had told them before they started. These conversations reveal patterns: what accelerates programs, what stalls them, and what separates the hospitals that thrive from those that struggle.
Here are five insights that keep surfacing in those discussions.
1. Commitment > Infrastructure
Most tertiary care hospitals serving regional populations are already positioned to do ECMO. Yet many delay ECMO programs because they believe they lack the necessary infrastructure.
The reality is that patient need and institutional commitment matter far more than perfect infrastructure. Programs have successfully launched with hospitals at varying capability levels. What matters most:
- Clinical leadership committed to the program’s success
- Evidence of patient need in your community
- Willingness to build what’s missing
The rest (equipment, EMR customization, monitoring protocols) can be developed or supplemented through partnership. Hospitals shouldn’t let “we’re not ready yet” prevent them from providing their community with life-saving care.
2. Network Access is One of the Most Underrated Benefits of Partnering
When hospitals partner with an experienced ECMO provider, they join a network of 50+ programs who’ve solved the problems they’re about to encounter.
Real examples from partner hospitals:
- A hospital implementing ECMO documentation in their EHR connects with a program that already built custom flowsheets and can share their build specifications
- Clinical teams troubleshoot complex cases with specialists who’ve managed hundreds of ECMO runs
- A team unsure how to properly code complex ECMO cases learns documentation requirements from programs that have optimized their billing workflows
This peer network is something hospitals building programs independently rarely have access to. There’s no way to Google the “what should we do when…” answers that come from lived experience across dozens of programs.
3. Flexibility is Non-Negotiable
ECMO programs evolve as teams gain experience and volume patterns become clear. What works in month three can look different by month twelve, and that’s normal and expected.
A program might budget for steady monthly volume, only to discover their census follows seasonal patterns that require different staffing approaches. A hospital might plan for a specific training curriculum, then realize their team needs more hands-on education or extended bedside precepting than what was initially scheduled. These aren’t necessarily failures of planning, but rather the natural process of learning how an ECMO program actually operates within a specific hospital’s reality.
Rigid plans create problems when reality diverges from projections. Flexible models allow programs to adjust in real time, based on what actually happens. This adaptability matters most in the early stages, when teams are still learning their true volume patterns and building experience with clinical scenarios they haven’t encountered before.
4. Speed to Launch = Speed to Impact (And Profitability)
The faster an ECMO program launches, the faster it delivers value, both in patient outcomes and financial performance.
Many hospital leaders have acknowledged they could have built their ECMO programs independently, but the timeline would have been significantly longer and the path to profitability extended by years. When programs launch faster, communities gain access to life-saving care sooner, and hospitals reach financial sustainability quicker.
For example, one hospital system had budgeted for a 5-year timeline to profitability when planning their ECMO program. Through partnership, the program launched in 90 days and became profitable within the first year. The difference wasn’t cutting corners, but rather in avoiding the months typically spent debating equipment vendors, developing policies from scratch, and building clinical competency in a therapy no one on staff has performed.
Programs that launch quickly leverage proven protocols, relationships, and staffing models that have already succeeded at other facilities. They bypass the trial-and-error phase that extends timelines and delays both clinical impact and revenue generation.
5. Being “First in the Region” Is a Bigger Win Than You Think
The value of launching the first ECMO program in your region extends beyond a press release. Most fundamentally, it means saving lives in your community that would otherwise be lost. Those survival stories—patients who walk out of your hospital who wouldn’t have survived without ECMO—create an impact that resonates throughout the region.
Beyond the clinical outcomes, launching an ECMO program signals to your community and to potential physician recruits that you’re a center of innovation and advanced care. The ripple effects extend across the organization. Cardiovascular surgeons choose facilities specifically because ECMO capability exists. Referral patterns shift as surrounding hospitals begin sending their most critically ill patients. Case Mix Index and hospital acuity scores improve, reflecting the complexity of care the facility can now manage.
Hospital leaders who’ve launched ECMO programs consistently describe it as one of the most meaningful initiatives they’ve undertaken. Not because of the revenue impact or strategic positioning, but because they can point to real patients in their community who survived because this capability existed when they needed it. That kind of impact is rare in healthcare administration—the ability to say definitively that lives were saved because of a decision made in a board room.
The Build vs. Partner Decision
For hospitals considering ECMO, the path forward comes down to timing, resources, and risk tolerance. Independent development is absolutely possible, it just takes longer, requires more upfront investment, and means solving problems that have already been solved at dozens of other facilities. Partnership offers a different timeline: faster launch, access to a network of established programs, staffing that scales with actual volume, and quicker path to financial sustainability.
Connect at Bridging Life
Integration Health will be at the Bridging Life Critical Care Symposium February 11-12 in Houston. This gathering brings together teams focused on caring for patients with severe heart and lung failure requiring ECMO, with sessions covering everything from device utilization and hemodynamics to infection prevention, mobilization, and team communication, all aligned with ELSO guidelines.
Our team will be supporting the conference in two ways: helping facilitate ECMO simulations throughout the event and staffing an exhibitor booth.
If you’re thinking about launching or growing an ECMO program, stop by. We’re happy to share what we’ve learned from 50+ program implementations and connect you with hospital leaders who’ve navigated these same decisions.
Find us at the simulations or visit our booth. Questions? Reach out at info@integration.health