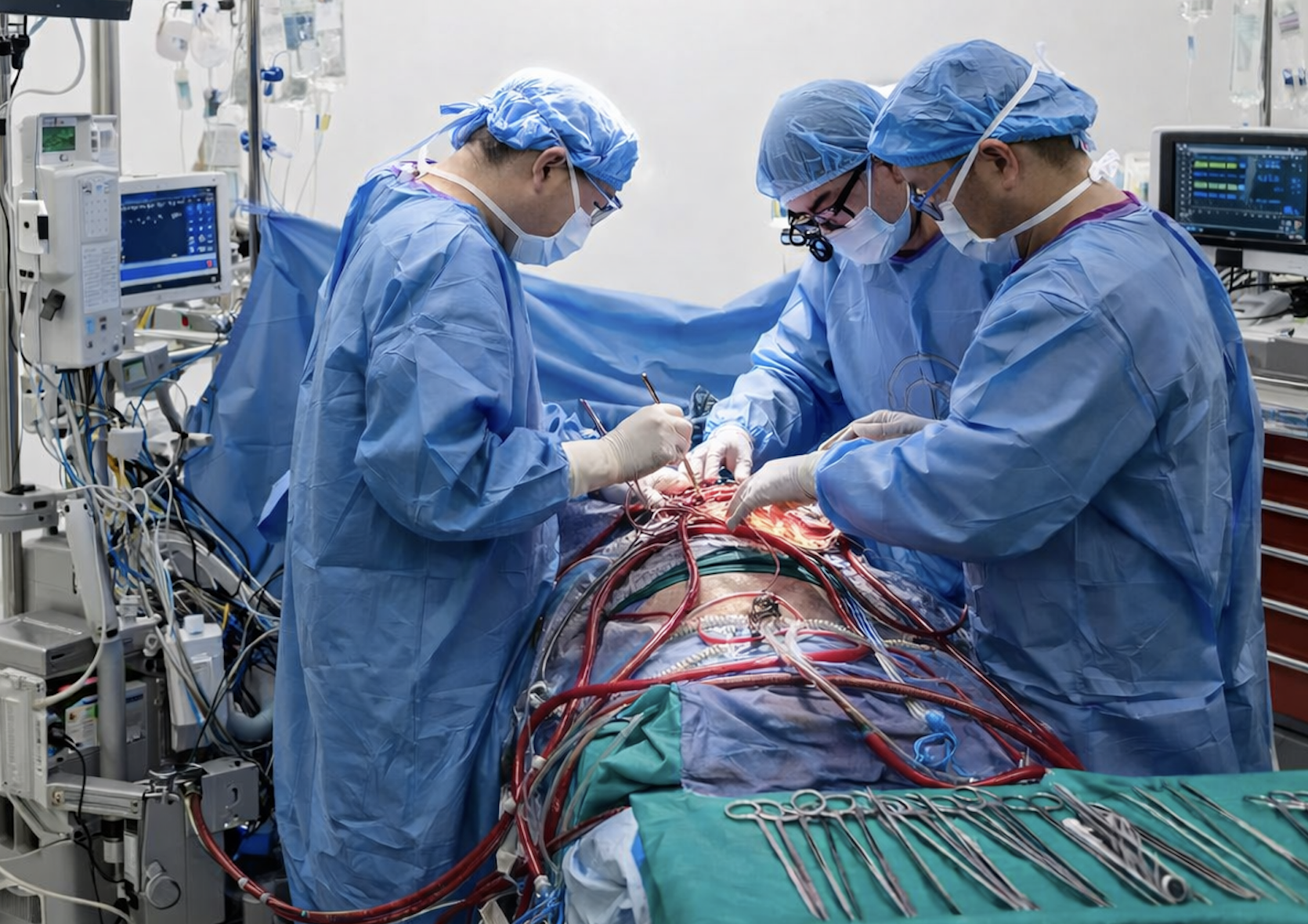
Extracorporeal membrane oxygenation (ECMO) is often considered a last resort, and thus, it has historically been used with caution in patients awaiting lung transplantation—especially older adults or those not yet listed for transplant. However, new research suggests that with the right approach, ECMO can be a viable and even life-saving bridge to transplant, regardless of when the patient is listed or how old they are.
Study Overview
In a recent retrospective study, researchers evaluated 50 patients who were placed on ECMO as a bridge to lung transplant. The median age of the group was 63 years old, an age group historically excluded from many ECMO programs due to assumptions about worse outcomes. Of the 50, half survived to transplant, and one-year survival for those transplanted was 88%—a rate nearly identical to the national average for all lung transplant recipients (87.8%).
Key Finding: Timing of ECMO and Listing Doesn’t Significantly Impact Survival
The study also explored whether outcomes varied depending on when patients were listed for transplant relative to ECMO cannulation. They found no significant difference in survival between those who were listed prior to ECMO versus those who were listed after ECMO had already begun—a model often referred to as “bridge to decision.” This finding is critical because it validates ECMO as a potential rescue option for patients who deteriorate before a formal transplant listing can occur.
The ability to stabilize patients on ECMO and later evaluate them for transplant gives clinicians more time and flexibility in complex cases. It also challenges long-held biases that older patients or those not yet listed are less likely to benefit. With the right infrastructure and a multidisciplinary team, outcomes can rival those of younger or less critically ill transplant candidates.
A Real-Life Example: Ben Askren
This research has timely real-world relevance in the remarkable story of former UFC fighter and MMA champion Ben Askren. Just weeks ago, Askren—who was previously in good health—was hospitalized with sudden, severe pneumonia that quickly progressed to respiratory failure. As his condition worsened, he was placed on a ventilator and then on ECMO.
At the time of his ECMO initiation, Askren had not yet been evaluated for a lung transplant. But rather than ruling him out, his medical team initiated the transplant evaluation process while he was already on ECMO—a textbook example of the “bridge to decision” approach described in the study. While Askren is younger than the patient population featured in the research, ECMO was used in the same way—not just to stabilize a patient, but to buy time, giving clinical teams the chance to assess whether a transplant is possible, and if so, to act swiftly.
Miraculously, Askren received a double lung transplant and is now in recovery. His wife, Amy, shared the news on social media, expressing deep gratitude to the donor family and the healthcare professionals who guided them through the ordeal. She noted that just five weeks prior, Ben had been walking around in perfect health—emphasizing how rapidly life can change, and how vital it is to have options like ECMO when the unthinkable happens.
Implications for the Future of Transplant Care
As ECMO technology continues to advance and more hospitals develop comprehensive programs, research like this study provides crucial evidence for expanding access to this life-saving therapy. The findings suggest that age alone shouldn’t disqualify patients from consideration, and that “bridge to decision” approaches can be successful when implemented by experienced teams.
For patients facing end-stage lung disease, these outcomes represent hope—evidence that even in the most dire circumstances, ECMO can provide a successful bridge to transplantation and long-term survival. As one researcher noted, the goal isn’t just survival to transplant, but ensuring patients can return home and live meaningful lives with their new organs.
The research reinforces what we at Integration Health already know: when properly implemented, ECMO programs can transform what were once impossible situations into stories of recovery and renewed life.