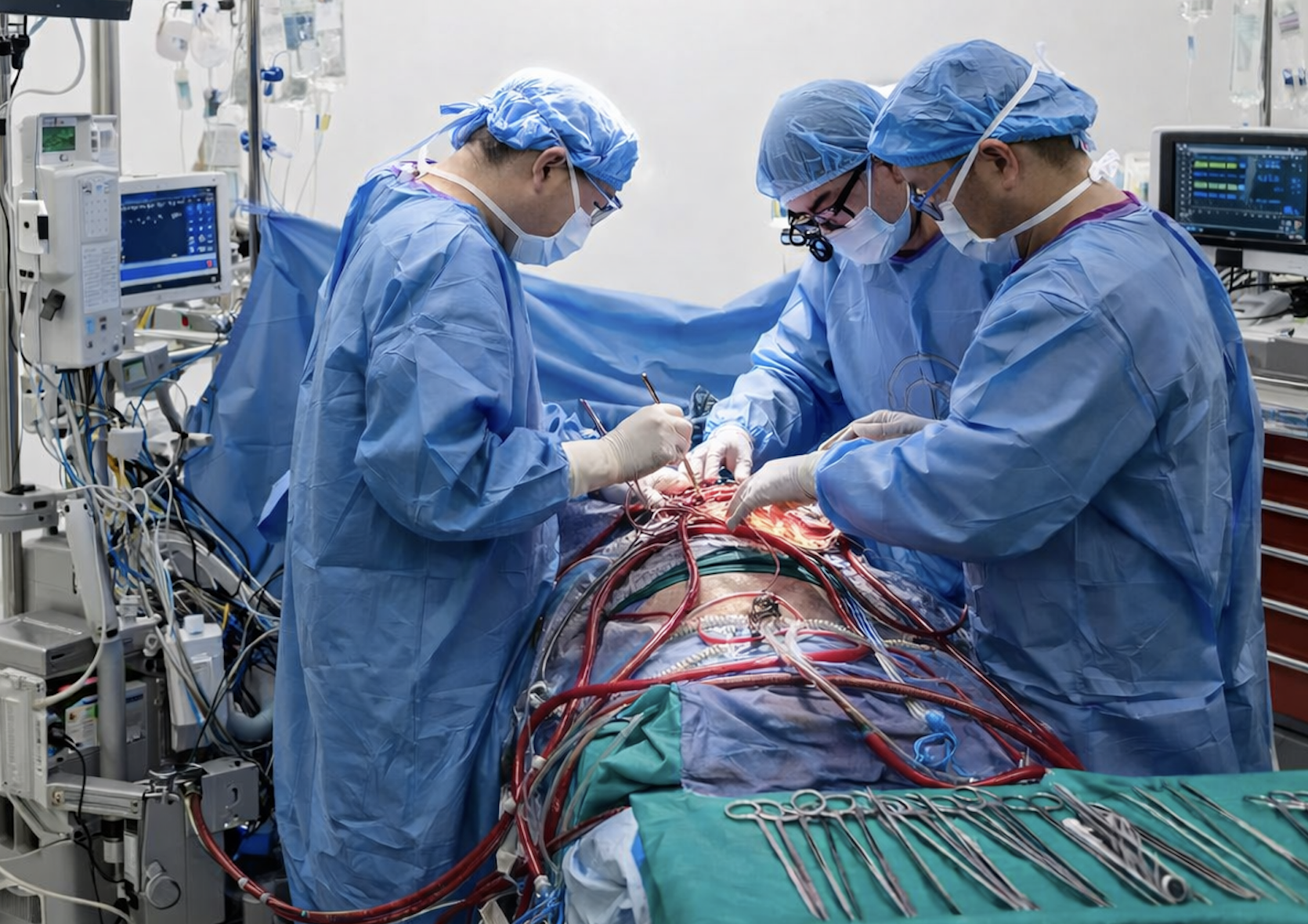
A recent study suggests liberal transfusion strategies may offer early survival benefits—but don’t change your practice just yet.
If you manage VA-ECMO patients, you’re probably following a transfusion protocol: whether it’s your institution’s order set, your program’s algorithm, or your attending’s preference. The threshold might be 7 g/dL, 8 g/dL, 9 g/dL, or somewhere in between, and it varies considerably across hospitals and even between providers at the same institution.
Despite how common this decision is (nearly 90% of VA-ECMO patients receive at least one transfusion), we don’t actually know which threshold is best. Different protocols exist not because the evidence points in different directions, but because the evidence barely exists at all.
What the Study Found
Researchers analyzed data from the OBLEX study, an international observational study of 534 VA-ECMO patients across 12 centers. Using advanced statistical methods to mimic a randomized trial, they compared outcomes between patients transfused at different hemoglobin thresholds:
- Restrictive strategy: Transfusion initiated at Hb ≤ 7 g/dL
- Liberal strategy: Transfusion initiated at Hb ≥ 9 g/dL
The findings revealed that patients managed with a liberal transfusion approach had improved survival compared to those managed restrictively—but this advantage only appeared during the first 2-3 days of ECMO support. The estimated survival benefit peaked at days 2 and 3, with differences of approximately 12-13% between groups. Beyond day 3, the survival curves converged and no difference was apparent.
This time-limited effect raises an important clinical question: is there something physiologically unique about the early phase of VA-ECMO that makes hemoglobin levels more critical?
Why the Early Benefit?
The authors propose a plausible mechanism: During the initial phase of VA-ECMO, if native cardiac function is severely impaired, ECMO flow may not fully compensate for reduced cardiac output. Combined with the lack of pulsatile flow, impaired endothelial function from shock, and potential tissue oxygenation problems, and you have a scenario where higher hemoglobin levels might genuinely improve oxygen delivery during the most critical early period.
The Evidence Gap We Can’t Ignore
However, one of the most important takeaways from this paper is that there are currently no randomized controlled trials examining transfusion thresholds specifically in VA-ECMO patients.
This study, while well-designed and hypothesis-generating, is ultimately observational. The authors are transparent about this, noting that their findings “should be interpreted as exploratory and hypothesis-generating, and do not support any immediate changes to clinical practice without further confirmatory research.”
The wide confidence intervals around their estimates (3-21% at day 2, 2-25% at day 3) reflect genuine uncertainty. We have interesting signals, but not definitive answers.
So What Should We Do?
This study doesn’t give us a definitive answer, but it does give us better questions to ask and a framework for thinking about transfusion timing in VA-ECMO.
For decades, the default in critical care was to transfuse liberally, often maintaining hemoglobin above 10 g/dL based on the assumption that higher levels meant better oxygen delivery. Then came the landmark TRICC trial in 1999, which randomized over 800 ICU patients to either restrictive (transfuse at Hb < 7 g/dL) or liberal (transfuse at Hb < 10 g/dL) strategies. The restrictive approach proved at least as safe, and possibly safer. Multiple subsequent trials reinforced these findings, and today, transfusing at 7 g/dL is standard practice for most critically ill patients.
But VA-ECMO patients weren’t included in these trials. As we know, these patients represent a unique physiology: severely compromised cardiac function, mechanical circulatory support, non-pulsatile flow, and often profound shock. Can we confidently extrapolate general ICU evidence to this population? This new study suggests maybe not—at least not in those critical first 48-72 hours.
Until we have definitive RCT data, clinical judgment guided by individual patient factors, hemodynamic parameters, and ECMO flow characteristics remains essential.