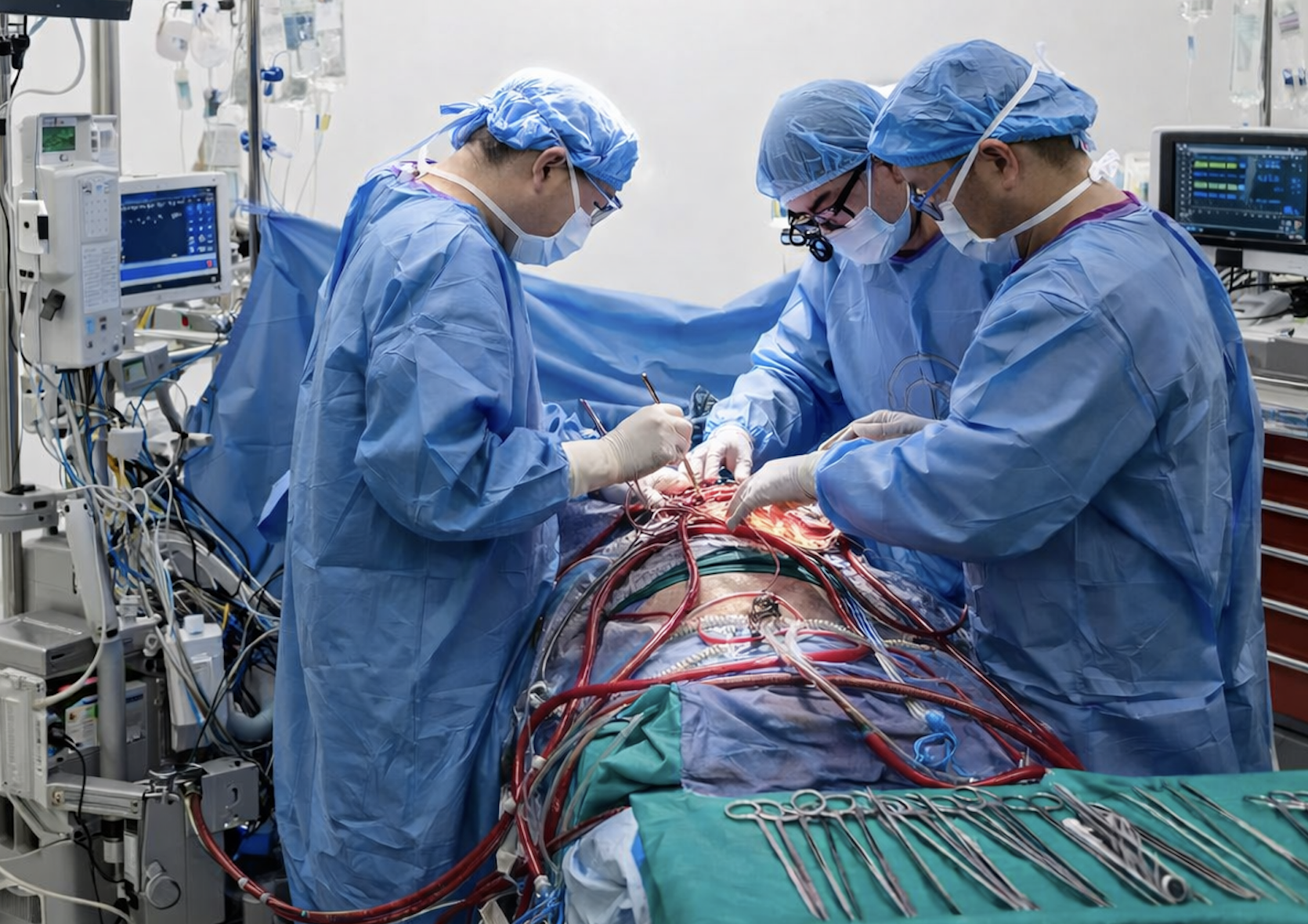
Every fall, cardiovascular program leaders face the same challenge: respiratory season is coming, ECMO demand will surge, but the timing and volume remain impossible to predict. This year, with overlapping flu, RSV, and COVID-19 circulating simultaneously, the pressure on ECMO programs has intensified—and so has the strain on the teams that support them.
For hospitals running ECMO programs, respiratory season isn’t just a clinical challenge. It’s a staffing puzzle that most programs struggle to solve.

Respiratory Season Drives ECMO Demand
From October through March, respiratory viruses circulate at peak levels just as colder weather drives people indoors, creating ideal conditions for viral transmission. This seasonal pattern drives a corresponding surge in severe Acute Respiratory Distress Syndrome (ARDS) cases. When conventional mechanical ventilation fails, ECMO becomes the next line of defense.
Studies show VV ECMO utilization tracks closely with influenza season, with ECMO demand rising significantly during months with higher influenza-like illness incidence. When flu season hits, ECMO programs feel it.
But here’s the challenge: while respiratory season creates a predictable increase in overall ARDS cases, individual ECMO runs remain unpredictable. A hospital might go weeks without an ECMO cannulation, then suddenly face three patients requiring support simultaneously, then drop back to zero as respiratory season ends. This feast-or-famine variability makes traditional staffing models nearly impossible to execute effectively.
The Staffing Dilemma: The Gap Between Need and Reality
Providing continuous bedside ECMO specialist coverage requires approximately 12-14 trained staff when accounting for shift coverage, time off, and safe staffing ratios. For hospitals running only a handful of ECMO cases annually, maintaining competency and availability of a full ECMO team is neither financially sustainable nor clinically practical.
ECMO is a highly complex therapy that requires training and regular hands-on experience to maintain proficiency. Staff who only manage ECMO a few times per year struggle to retain the sharp clinical judgment and technical skills this demanding therapy requires. At the same time, dedicating 12-14 specialists to a low-volume program means those providers will rarely perform ECMO, creating a cycle where skills inevitably decay.
The problem compounds during respiratory season. When ECMO census unexpectedly doubles or triples, programs face impossible choices:
- Pull staff from other units to help manage ECMO patients—but ECMO is so highly specialized that expecting ICU nurses or respiratory therapists without specific ECMO training to safely manage these critically ill patients is unrealistic and potentially dangerous
- Pull perfusionists from the OR, which compromises the cardiovascular surgery program and creates conflicts between competing critical services
- Stretch existing ECMO specialists beyond safe limits, risking both clinician wellbeing and patient outcomes
- Transfer patients to other facilities, losing both the patient relationship and significant revenue
Traditional locum staffing agencies can’t solve this problem. ECMO expertise is too specialized, the credentialing process too lengthy, and the clinical need too immediate. By the time a traditional agency identifies, credentials, and deploys an ECMO specialist, the surge has often passed—or the program has been forced into one of the difficult compromises listed above.
Respiratory season amplifies every aspect of this dilemma. The predictable increase in ARDS cases creates sustained pressure, but the unpredictable timing of ECMO cannulations means programs can’t simply “staff up” for a defined period. They need sustained readiness with the flexibility to scale immediately when census spikes.
The Integration Health Solution: Ready When You Need Us
Integration Health was built specifically to solve this challenge. Rather than asking each hospital to maintain a full ECMO team for unpredictable demand, we maintain a deep bench of specialists who stay sharp by working regularly—and we deploy them to hospitals nationwide within 24 hours of a patient being placed on ECMO.
Here’s how the model works:
Every day, we have 20+ ECMO specialists and perfusionists ready to deploy nationwide, all exclusively dedicated to ECMO and perfusion services. These aren’t generalists who do occasional ECMO—they’re experts who average 11.5 ECMO shifts per month. That means when they arrive at your facility, they bring current, hands-on experience with the therapy.
Guaranteed availability within 24 hours. When your patient is cannulated, we deploy a specialist to your facility. Once we arrive, we’re committed to supporting that patient until ECMO is discontinued—whether that’s three days or three weeks. Your program maintains continuity of expert care without scrambling to cover shifts.
We work alongside your existing team. Our specialists integrate seamlessly with your intensivists, nurses, and respiratory therapists, filling gaps where needed. They bring ECMO expertise while respecting your facility’s protocols and culture. For many programs, this partnership model also provides valuable training opportunities for permanent staff.
No year-round cost burden. You pay for coverage only when you have ECMO patients. This means you can offer ECMO to your community without maintaining 14 full-time specialists or compromising on expertise when census is low.
This model addresses both the predictable pressure of respiratory season and the unpredictable nature of individual ECMO runs. Whether you’re facing a sustained surge of ARDS cases or a sudden spike in census, Integration Health ensures your program can respond with confidence.
Building Long-Term Program Success
Integration Health is also invested in helping programs build sustainable, independent capabilities over time. We offer comprehensive ECMO training, from accredited online courses to hands-on simulation, ensuring your permanent staff develops and maintains proficiency.
We also provide program optimization services, helping hospitals refine patient selection criteria, update protocols, and optimize revenue cycle management to ensure your ECMO program captures the reimbursement it deserves. Whether you need full coverage now with a path toward independence, or ongoing support for complex cases and surges, we tailor our partnership to your program’s specific goals.
Respiratory Season Is Here. Is Your ECMO Program Ready?
Respiratory viruses are already circulating across the country. ARDS cases are climbing. And somewhere in your region right now, there’s a patient who will need ECMO in the coming weeks, possibly at your facility.
Does your program have the staffing model to handle that pressure without compromising patient care or forcing impossible choices between competing priorities?
With Integration Health, expert ECMO coverage is always available, specialists maintain sharp skills through regular practice, and your program pays only for the coverage you actually use.
Ready to learn more about how Integration Health can support your ECMO program?
Contact us today to discuss your program’s specific needs and how our nationwide specialist network can provide the coverage and expertise your patients deserve—during respiratory season and throughout the year.